Do pedometers do more harm than good?
Speaking at the annual meeting of the American Association for the Advancement of Science (AAAS) in Boston, Dr Greg Hager, professor of computer science at Johns Hopkins University, warned that obsessing over achieving the basic philosophy of 10,000 steps daily may lead people to chase over-ambitious goals and, as a result, do more harm than good.
Why 10,000 steps?
The leading expert pointed out that the target appears to be a relatively arbitrary figure. “Turns out in 1960 in Japan they figured out that the average Japanese man, when he walked 10,000 steps a day, burned something like 3,000 calories and that is what they thought the average person should consume. So they picked 10,000 steps as a number.”
Are pedometers recommended for monitoring physical activity?
Physical activity monitors or trackers, such as pedometers, have gained increasing popularity. When used appropriately, they serve a useful purpose by providing objective measures in activity and provide constant encouragement for people to move more. Pedometers can be a useful tool to create general awareness of activity levels by counting the number of steps taken. However, some users may become fixated on the “10,000-step rule”.
Should I be counting steps?
Rather than being fixated on reaching 10,000 steps a day using a pedometer, it can be used to track the average daily step count, then applied to setting appropriate goals. For a generally healthy individual looking to increase activity in daily routine, gradually increasing the number of steps may be a good way to start. While 10,000 steps per day may have a positive effect on health, it is important to note that the target is not based on science-based evidence. In addition, achieving 10,000 steps may not be feasible for everyone.
Are pedometers recommended for monitoring physical activity?
Relying solely on pedometers in measuring physical activity is unreliable. For one thing, it does not provide important measurement parameters such as duration and intensity. This highlights an important medical risk associated to the application of pedometers and consumer activity trackers in clinical applications.
Activity monitoring for research or clinical applications needs to be precise and validated. For this purpose, accelerometer-based activity monitors, such as the MOX, is used extensively. The MOX has been used to investigate the correlation of physical activity or sedentary behaviour to disease outcomes, as well as to monitor older adults and individuals with chronic conditions in the home and community settings. By customising accelerometer-based algorithms that accurately classify physical activity levels and/or posture such as sitting or lying for specific populations or individuals, reliable and valuable insights into real-world physical activity or movements can be obtained. Combined with activity goal settings, the activity monitor can be used to support translational care interventions. Furthermore, this information enables medical professionals to monitor and support their patients and provide more precise medical advice.
To find out more about the MOX Research system, click here.
Do you have ideas for physical activity monitoring? Feel free to contact us and discuss your ideas!
EU Falls Festival 2017 - Insights on physical activity monitoring
On May 8 and 9 2017, the annual European Falls Festival was held at the Amsterdam Medical Centre, with the theme “Developing Collaborations across Professions and throughout Europe”. Leading multi-disciplinary professionals were brought together at the highly respected conference to discuss the research and innovation in the study and implementation of falls prevention in older people. The Accelerometry.eu team was present to exhibit our latest products, including the MOX accelerometry sensor. The topic of “fall technologies”, which can be classified in four domains: fall detection, fall assessment, fall prediction and fall intervention, were addressed in many presentations. Wearable physical activity monitoring technologies were highlighted in many presentations. An overview of interesting topics is included below:
Physical activity monitoring
Being physically active in a safe manner
Valpreventie.be provides useful information on fall prevention methods and strategies for older persons and caregivers. The theme of the national Belgian Fall Prevention Week was “Stay Active, Do It Safe”. On being safe while staying physically active, topics relevant to daily physical activities were brought to attention. These include footwear, vision, medication, dizziness, food and home/environment safety. Physical activity monitors with fall detection algorithms can be used to detect falls and provide additional safety by calling for help if appropriate.

After hospital discharge
Bianca Buurman, Professor of Transitional Care at the Amsterdam Medical Centre, highlighted the importance of early mobilization and physical activity 10-15 days following hospital discharge. There is a potential for eHealth activity monitoring tools to support transitional care interventions. By encouraging appropriate physical regimens in transitional care, the long term risk of falls due to functional decline may be reduced.
Novel technologies for successful fall prevention
Luca Palemerini, Research Fellow at the University of Bologna and Adjunct Professor of the Biomedical Signals & Data Processing course of the Master degree in Electronic Engineering, provided a stimulating overview of technology for fall detection and fall risk estimation using wearable sensors and data mining. The opportunities for wearable accelerometers are:
- fall risk assessment
- activity monitoring
- intervention / fall prevention trainig
- assisted living
for more information about MOX Accelerometry or accelerometer-based algorithms.
Optimal placement of accelerometers for fall detection in the elderly
Fall detection in the elderly
Falls are a major public health problem in the elderly and is a leading cause of unintentional injury and deaths in the elderly population worldwide. A fall episode can have profound implications on their independence, health and overall quality of living, imposing additional socio-economic burdens. Many complications from an unattended fall could be prevented if prompt help was received or properly detected in situations of daily life. Over the years many fall detection devices have been proposed for the elderly, but many do not provide an effective solution. The most promising angle of fall detection seems to be the use of accelerometers. However, there are many different approaches on placement of accelerometers for fall detection, and it seems uncertain which one is preferable. Generally, there are a few evaluation criteria and consideration factors.
Criteria of fall detection systems
The placement site can largely affect the four possible situations of a fall detection system (Noury, N., et al.):
- true positive (TP), a fall occurs and the system correctly detects it;
- false positive (FP), the system declares a fall event, but it did not occur;
- true negative (TN), a normal fall-like movement is performed, the device does not declare a fall;
- false negative (FN), a fall occurs, but the system does not detect it.
Three criteria are proposed to evaluate the reliability of a fall detection system (Abbate S., et al.):
- sensitivity = TP/(TP + FN), the ability to detect all real falls;
- specificity = TN/(TN + FP), the ability to detect only real falls;
- accuracy = (TP + TN) /(TP + FP + FN + TN), which is the proportion of true results in the considered data set
Aside from the capacity of the fall detection system, usability is also often considered as it is a fundamental factor for real adoption of a fall detection system.
Review of accelerometer placement strategies
A brief review on promising accelerometer placement strategies in present literature was performed by a current student from Maastricht University as part of Masters coursework. Three studies stood out when validity was compared based on three attributes: sensitivity, specificity and usability.
Study #1 (Kangas M., et al.)
The first study used three sensors (forehead, waist and wrist), which achieved a specificity and sensitivity of 100% and 98% respectively. When the data gathered by the wrist sensor was excluded, reliability was only slightly lower. Despite a high validity, the placement of a sensor on the forehead makes this an undesirable option for use in daily life.
Study #2 (Gjoreski H., et al.)
The second study used four sensors (sternum, waist, thigh and ankle; and found a specificity and sensitivity of 99% and 97.8% respectively. This sensor placement would probably be preferable to the one used by Kangas as it is less obtrusive. However, it would require regular replacement of four sensors which likely lead to low compliance, hence defeats the purpose of using this placement strategy for accurate fall detection.
Study #3 (Abbate S., et al.)
Lastly, the third fall detection system included a smartphone-based setup. It was found that data from a single sensor on the thigh analysed by the smartphone, in conjunction with the smartphone’s integral accelerometer, achieved a specificity of 100% but a relatively low sensitivity of 96.3%. When using only the smartphones integral sensor without an additional sensor, both sensitivity and specificity were too low to qualify as accurate fall detection. The disadvantage of using the smartphone for fall detection in the study is the need to be carried (within range of 3 meters) and to remain charged at all times. This is not always feasible. Furthermore, carrying a smartphone enables the individual to contact relatives or caregivers for assistance in the event of emergency if a fall should happen. In this context, the possibility of using a small external sensing unit can greatly reduce the intrusiveness of the system.
Conclusion
The author concluded that there is currently no clear optimal placement that will outperform the others in every situation. For home use, the smartphone based setup would likely have the populations’ preference, although there is a high chance of the phone being out of reach when it is most needed, when compared to accelerometer-only setups. For research purposes the placements used by Kangas and Gjoreski would have the upper hand based on sensitivity, although gathering subjects for field research may be easier when only one sensor and a Smartphone are required.
Comments
The proposed placement strategies and accelerometers for fall detection in the elderly are numerous, and reliability may be comparable. However, fall detection systems based on wearable sensors are reliant on user compliance (remembering to wear the device and choosing to wear the device). Therefore, it is expected that systems with multiple sensors will be less favourable and result in lower compliance in the elderly.
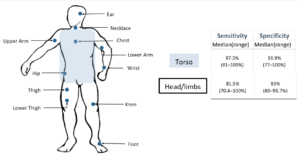
Fall detection systems with single sensors placed on the torso is the most common, as revealed revealed in a systematic review (Chaudhuri et al., 2014). Illustration on the right shows the sensitivity and specificity of such systems with respect to the sensor location. Devices placed on the torso had a sensitivity and specificity with a median sensitivity and specificity of 97.5% (81–100%) and 96.9% (77–100%) respectively (Chaudhuri et al., 2014). Whereas, devices placed around the head and limbs had a lower median sensitivity and specificity of 81.5% (70.4–100%) and 83% (80–95.7%) respectively. Those involving multiple sensors had a median sensitivity of 93.4% (range 92.5–94.2) and a median specificity of 99.8% (range of 99.3–100).
Although many fall detection systems show high sensitivity and specificity in simulated research settings, it is important to take note that it may not reflect the same reliability in real-world situations. As algorithms are optimized to the test situation, real-world tests would be a more rigorous indicator of the device’s reliability. However, few have been performed. Therefore, more real-world tests may be necessary to prove the efficiency of these systems before implementing it as a feasible solution for fall detection in the elderly.
References
Abbate S, Avvenuti M, Bonatesta F, Cola G, Corsini P, et al. A smartphone-based fall detection system. Pervasive and Mobile Computing. Vol 8 (6). Dec 2012.
Gjoreski H, Lustrek M, Gams M. Accelerometer Placement for Posture Recognition and Fall Detection. Intelligent Environments. 2011.
Kangas M, Konttila A, Lindgren P, Winblad I, Jamsa T, et al. Comparison of low-complexity fall detection algorithms for body attached accelerometers. Gait & Posture. Vol 28 (2). Aug 2008.
Noury, N., Rumeau, P., Bourke, A. K., ÓLaighin, G., & Lundy, J. E. (2008). A proposal for the classification and evaluation of fall detectors. Irbm, 29(6), 340-349
Acknowledgements
The review of accelerometer placements in the current literature was contributed by Gerard van der Linden, a current Masters student in Maastricht University’s Faculty of Health, Medicine and Life Sciences (FHML).
for more information about MOX Accelerometry or fall detection algorithms.
Quantifying free-living sedentary behaviour using activity monitors
Assessing physical activity
Quantifying physical activity, or lack thereof, have been used to analyse sedentary behaviour in order to understand physical activity and disease outcomes, as well as define the effectiveness of intervention strategies. Physical activity has previously been assessed by means of self-reported measures such as questionnaires and interviews, especially in larger population studies. However, such self-reported measures can report bias in the study. With advancement in technology, wearable activity monitors are increasingly being used to objectively quantify free-living sedentary behaviour. Furthermore, they are generally small, lightweight, portable, non-invasive and unobtrusive.
The study
A recent large population study (2,497 individuals) published in the journal Diabetologia on 2 February 2016 (1) was one of such studies undertaken to measure free-living sedentary behaviour using wearable activity monitors. The study, led by first author Julianne van der Berg and senior author Annemarie Koster from Maastricht University, looked at the amount and patterns of sedentary (sitting or reclining) behaviour in relation to type 2 diabetes and the metabolic syndrome. It was performed within The Maastricht Study, an extensive phenotyping study of adults that focuses on the etiology of type 2 diabetes and its complications and comorbidities.
Results
The study participants with Type 2 Diabetes spent less time stepping and had less moderate intensity activity but the most significant risk factor is the increased time spent sedentary (sitting/lying). It was concluded that an extra hour of sedentary time was associated with a 22% increased risk for type 2 diabetes and 39% increased risk for the metabolic syndrome. These results suggested that sedentary behaviour may play a significant role in the development and prevention of type 2 diabetes.
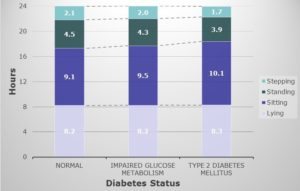
Fig. 1 Time (hours) spent in primary daily activities according to glucose metabolism status. (Adapted from van der Berg et al., 2016) (1)
Activity monitors
There are activity monitors that have been developed for research purposes and more specifically, for accurately distinguishing sedentary behavior. The Glasgow-based PAL Technologies’ activPAL™ activity monitor was chosen by the researchers in the Maastricht Study. Similarly, the MOX activity monitor has proven high accuracy in determining free-living physical activity behavior and assessing different activity intensities in healthy and chronically ill patients (chronic obstructive pulmonary disease, type 2 diabetes or mitochondrial disease) (2, 3). Furthermore, the MOX activity monitor is waterproof and can be adhered directly to the skin on the thigh 24/7 for 8 days by a patch. Using accurate, reliable and objective activity monitors is an advantage as advances in accelerometry technology have allowed low power consumption, easy setup, and unobtrusive design to provide a promising tool for monitoring free-living physical activities.
Click here to the article by van der Berg et al. published online in the journal Diabetologia, 2016.
REFERENCES
- van der Berg JD, Stehouwer CDA, Bosma H, van der Velde JHPM, Willems PJB, Savelberg HHCM, et al. Associations of total amount and patterns of sedentary behaviour with type 2 diabetes and the metabolic syndrome: The Maastricht Study. Diabetologia. 2016;59(4):709-18.
- van der Weegen S, Essers H, Spreeuwenberg M, Verwey R, Tange H, de Witte L, et al. Concurrent Validity of the MOX Activity Monitor Compared to the ActiGraph GT3X. Telemedicine and e-Health. 2015;21(4):259-66.
- Koene S, Dirks I, van Mierlo E, de Vries PR, Janssen AJWM, Smeitink JAM, et al. Domains of Daily Physical Activity in Children with Mitochondrial Disease: A 3D Accelerometry Approach. Berlin, Heidelberg: Springer Berlin Heidelberg. p. 1-11.
For more information about The Maastricht Study:
https://www.demaastrichtstudie.nl/research
For further information about the Maastricht Study, please contact :
 Anniemarie Koster
Anniemarie Koster
Associate Professor
Associate Professor Programme: Inequity, Participation and Globalisation (IPG)
Sociale Geneeskunde, School for Public Health and Prim Care, Fac. Health, Medicine and Life Sciences
Exercise Does Not Negate the Harmful Effects of Inactivity
Exercise is healthy, but an hour per day cannot fully compensate for the negative effects of excessive sitting and inactivity during the rest of the day.
It is generally known that exercise is beneficial for health and in reducing the risk of metabolic diseases such as diabetes and cardiovascular diseases. Unfortunately, many adults do not reach the current physical activity guidelines (150 minutes of moderate to vigorous physical activity per week). Moreover, we sit too much. In the car/bus on the way to work, at work behind our desk and at home in front of the television or computer. Inactivity, especially excessive sitting, is a major implicator of metabolic diseases and has been branded the “new smoking” for its supposed health risks. Whether this statement is true is inconclusive based on current research, but one thing most researchers do agree: too much sitting is unhealthy.
Decreasing sitting time by moving more and fitting physical activity into your day is one way to get started. Other than a bout of exercise a day, an easy alternative is to increase movement in our daily activities, such as housework, gardening, walking or cycling as a mode of commute and taking the stairs. A recently published study by Duvivier et al. (in scientific journal Plos One) suggested that one hour of daily physical exercise cannot fully compensate for the negative effects of inactivity on risk factors for cardiovascular disease (insulin level and plasma lipids) if the rest of the day is spent sitting.
The Study
In this study, eighteen healthy young subjects, age 21±2 year old of normal BMI followed one of three randomly assigned physical activity regimes for four days. In the sitting regime, participants were instructed to sit 14 hr/day. In the exercise regime, participants were instructed to sit 13 hr/day and to substitute 1 hr of sitting with 1 hr of vigorous supervised bicycling. Lastly, participants in the minimal intensity physical activity regime were instructed to substitute 6 hrs sitting with 4 hr walking and 2 hr standing. All regimes were instructed to walk 1 hr/day, stand 1 hr/day and spend 8 hr/day sleeping or supine. The exercise and minimal intensity physical activity regime had the same daily energy expenditure. During the four days of regime, physical activity monitors were continuously worn (24 hours a day) by the participants.
Figure 1. Time spent on different activities per regime.
Graphical overview of the three regimes followed by the participants and time spent in different activity categories (sleeping, sitting, standing, cycling and activity (walking).
Results
Results of the study showed that reducing inactivity by increasing the time spent walking/standing is more effective in lowering blood cholesterol and lipid levels, when energy expenditure is kept constant. Moving more everyday and reducing prolonged sitting time is much more effective than a bout of one hour intensive cycling exercise. It also demonstrated that the negative effects of extensive sitting on our health cannot be compensated by an hour of exercise per day. Therefore apart from including exercise in our lifestyle, health advice should also focus on decreasing sedentary time and moving more.
One of the strategies to keep track of daily movements is the use of an activity tracker. Physical activity trackers have gained popularity to assist individuals in monitoring their level of activity and reaching their daily activity goals.
Reference:
Duvivier BMFM, Schaper NC, Bremers MA, van Crombrugge G, Menheere PPCA, Kars M, et al. (2013) Minimal Intensity Physical Activity (Standing and Walking) of Longer Duration Improves Insulin Action and Plasma Lipids More than Shorter Periods of Moderate to Vigorous Exercise (Cycling) in Sedentary Subjects When Energy Expenditure Is Comparable. PLoS ONE 8(2): e55542.
Download the article here.
For more information about this study, please contact:

Bernard Duvivier, MD
Department of Internal Medicine
Department of Human Movement Sciences
Maastricht University Medical Centre
Maastricht, The Netherlands
bernard.duvivier@maastrichtuniversity.nl